自己由来および同種他家由来の細胞療法への期待と課題
August 25, 2021
Marie-Ange Kouassi
The promise of cell therapies as personalized medical interventions is immense, providing breakthroughs in curing diseases with inadequate or no existing treatment options, regenerating impaired tissues, and targeting pathologies for which traditional treatment has limited efficacy. Current cell therapies in development fall under two main categories—autologous and allogeneic. Each category presents a diverse range of challenges related to development and bedside application. A deeper understanding of these challenges is required to identify the appropriate solution to optimize the development process and match the most suitable therapy to a particular patient. In this article, we describe the main challenges faced by companies operating in this rapidly evolving scientific field when converting discoveries into life-changing precision therapies for patients.
Cell Therapy Product Development
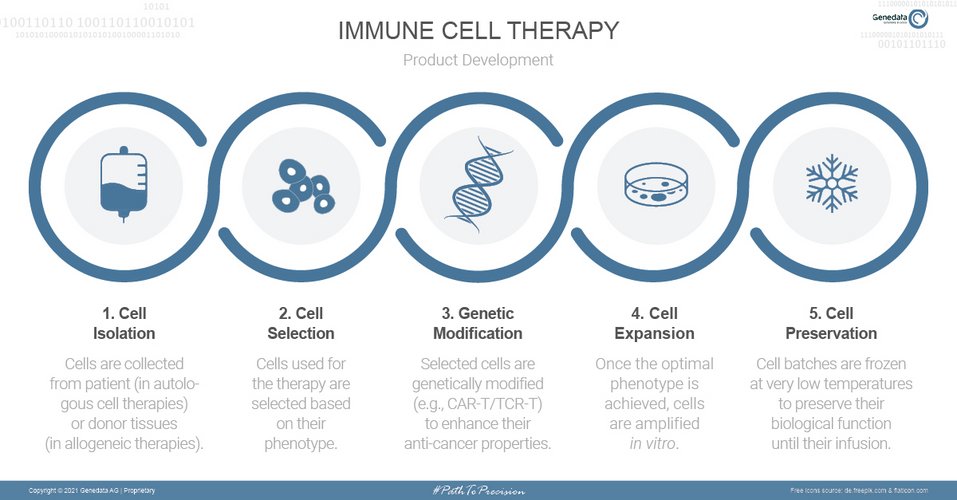
Cell therapies involve the use of stem, progenitor, or differentiated cells harvested from and reintroduced into the same patient (autologous) or harvested from a healthy donor and infused into a patient (allogeneic). Following the collection of these cells, phenotypic selection, genetic manipulation, and in vitro cell expansion steps are performed before administration to patients.
As the cells are sensitive to minor changes in their environment or variations in the process chain, this process of transforming them into effective therapeutic products is highly complex, requiring a high level of diligence.1
The cell therapy product development process is unique and depends on the selected approach (autologous or allogeneic). As each approach comes with its limitations, it is important to consider these early on, to enforce improvements that improve the efficacy of a treatment for a particular medical intervention.
Autologous Therapies
As they are derived from a patient, autologous cell therapies provide many benefits yet present several challenges which prevent them from fulfilling their maximal benefit. One of the key challenges of the autologous cell therapy production model is product stability, as these therapies exhibit a short half-life of as little as a few hours ex vivo.2 As a result, production in a manufacturing facility—which involves genetic modification, expansion, and cryopreservation, needs to take place close to the clinical environment, where cellular harvesting and/re-administration occurs. It is paramount that the entire development process is conducted very efficiently: not only to preserve product integrity and volume but most importantly, to treat patients whose prognosis worsens over time.
The effort required to develop autologous cell therapy products is considered worthwhile due to its immunological advantages. Using a patient’s own cells reduces the chances of an immunological reaction against the final therapy and life-threatening reactions such as graft-versus-host disease (GvHD), which can be observed with allogeneic therapies.3,4 GvHD is an immune condition that manifests when the immune cells of the donor (the graft) attack a patients’ (the host) cells. This condition can range from acute to chronic/life-threatening and comprises inflammatory symptoms such as enteritis, and dermatitis. Since immune compatibility is critical in all areas of transplantation, autologous approaches such as using a patient’s somatic cells are attractive as they do not require immunosuppression prior to treatment.5 A good example of such an approach is the use of a patient’s somatic cells for reprogramming into induced pluripotent stem cells (iPSCs), which can differentiate into multiple cell types for engraftment and tissue regeneration. Such iPSCs have been developed to combat Parkinson’s Disease by engraftment to regenerate midbrain dopamine neurons.6 Autologously derived cell therapies also stand a better chance of persisting in a patient’s body for months or years, eliciting long-term responses.
To treat highly prevalent diseases using cell therapies, scaling up production is essential. This is challenging when it comes to autologous cell therapy as each therapy is unique to a patients’ cellular profile, genotype, and phenotype (e.g., HLA type) as well as demographic (e.g., age) and medical history. These differences need to be considered as they may affect cell availability, viability, or therapeutic properties. For instance, it is important to consider whether patients suffering from a medical condition have a genetic tendency for the disease. If this is the case, treating a patient with cells that are genetically predisposed to the disease may have no therapeutic benefit. Screening patients diligently to identify those who will benefit from autologous therapies as well as investigating whether cell manipulation will overcome any genetic predisposition to the target disease are essential.7 There is also a substantial level of heterogeneity between production batches because of the above-mentioned differences, creating difficulties in maintaining quality attributes (e.g., cellular integrity and phenotype) and reducing the safety and efficacy of a treatment.8
Manufacturing and Logistics
In addition to the difficulties in harvesting an abundant number of high-quality cells for engineering, the logistics are complex as they involve two clinical procedures (isolation and re-infusion). It is important that the procedures are well-timed and that the high risk of cross-contamination is mitigated. For example, while manufacturing autologous cell therapy, removing malignant cells from the source material is crucial as these can put a patient at risk of relapse following re-infusion.9 Time is also a critical factor. The turnaround time from cell isolation to re-infusion of modified cells into the same patient can be several weeks, which is too long for some diseases, especially if the cell therapy is a measure of last resort.
Due to the high level of personalization required during the development of autologous therapies, the cost of delivering them to patients is extremely high. Therefore, such therapies are referred to as following a “service-based” model. With insurance and healthcare systems consistently striving to reduce costs, such a model is unattractive, and cheaper traditional treatments are preferred. By increasing production efficiency, enhancing specificity, quality, and integrity while developing efficacious production processes, costs can be reduced, while providing effective autologous cell therapies to patients.7 To facilitate this, close collaborative relationships with data management and analytics system providers are required. These partnerships will help to identify critical aspects of production science that allow for more successful product design.
Allogeneic Therapies
Allogeneic cell therapies follow the same overall production process as autologous therapies with the critical difference being that the cells are derived from healthy donors (see infographic). This carries with it many advantages especially the possibility to produce “off-the-shelf” products readily available to patients and for the treatment of a wider range of pathological conditions. The cells used for therapies are harvested from a single source, genetically engineered to elicit a desired therapeutic response, and stored in a cell bank until they are shipped to patients when required. As a result, patients receive the treatment on demand from the manufacturing facility, a time-saving that is particularly important in the context of rapid disease progression.
As the cells originate from healthy donors—rather than patients who may have been pre-exposed to treatment such as chemotherapeutic agents—it is usually easier to obtain a product of improved quality when developing allogeneic cell therapies. The harvested cells can also be pre-selected for the best quality as numerous batches originate from the same donor, enabling greater consistency. In the situation where a patient requires another treatment course, an identical batch can be rapidly delivered.
The use of multipotent stem cells is especially attractive for allogeneic processes as multiple indications could be addressed with a singular product. Allogeneic hematopoietic stem cell (HSC) transplantation has already shown promise in treating secondary skin neoplasms, follicular and indolent B cell lymphomas (slow-spreading and asymptomatic), and metastatic breast cancers.11-14 Allogeneic stem cell therapies have also been shown to be capable of stimulating early production of host paracrine factors to aid tissue remodeling/regeneration, so even transient dosing without permanent cell integration has medicinal value. 14
Key Considerations for Allogeneic Cell Therapy Development
To the biopharmaceutical industry, the allogeneic model is more financially appealing as it does not involve the costly service component of autologous therapies. Additional advantages include the potential to scale production and selection of the donors with the highest cell potency. The main consideration for manufacturing is the ability to achieve high-quality cells in sufficient quantities to treat millions of patients at a sustainable cost per dose and indication. Allogeneic cell therapies are also advantageous as more complex manipulation can be performed in a controlled manner with quality assurance standards. The possibility to leverage automation and scale up the manufacturing process, reduces the cost of these cell products, allowing companies to offer a competitive price.9
Immunological Reactions
Although allogeneic cell therapies have many advantages, there are still two major challenges to overcome: immunological rejection and elimination.4 Immunological rejection of administered cells can occur due to the host’s identification of donor cells as foreign. The elimination of donor cells poses a major challenge whereby the cell therapy may be rapidly removed before it can provide therapeutic or regenerative benefits to the patient.15 In fact, an ongoing immunological response may lead to immunological memory against administered allogeneic cells, making redosing to overcome the loss of benefit, less therapeutically effective after the first dose.
These challenges may be addressed by using immunosuppressant therapies or through further genetic engineering of donor cells. However, immunosuppression carries with it many side effects, including increased risk of infection, kidney and liver toxicities, metabolic disturbances, and hypertension.16 Moreover, loss of control over cell division in transplanted allogeneic stem cells may progress to a type of cancer or teratoma. Permanent cell integration/differentiation is required to deliver optimal therapeutic results and has prompted investigation into other avenues for overcoming these challenges. Mesenchymal stem cells (MSCs), for instance, have the major benefit of being immune-privileged, enabling them to survive for extended/indefinite periods without acute rejection. During transplantation of such treatment, patients may not require immunosuppression co-therapy.17
General Challenges of Cell Therapies
Besides adverse effects resulting from immunological rejection, there are additional challenges preventing cell therapies from being successfully and widely incorporated into personalized disease management plans (see infographic). These challenges include the risk of toxicity-related events such as cytokine release syndrome (CRS) and CAR-related encephalopathy syndrome (CRES), lack of response, or a reduction in efficacy over time (causing relapse), as well as the inability to penetrate certain tumor types. Solutions are required that address these challenges and enable cell therapies to be applied to a broader range of therapeutic indications.
Toxicity Observed with Cell Therapies
As adoptive cell therapies (ACTs) often induce an increased release of cytokines, this rapid surge can lead to CRS within 1 to 14 days after cell infusion, which initially manifests as fever, myalgias, and fatigue. This condition, also known as a “cytokine storm”, can progress to a life-threatening status with multiple lethal organ dysfunctions.18,19 The standard treatment for CRS is an IL-6 receptor antagonist, Tocilizumab, and in refractory patients, corticosteroids may be prescribed to suppress inflammatory responses.19 However, as it may induce T cell apoptosis or suppress cellular function, its effects on the efficacy of the ACT itself should be considered. Although some patients who suffer from CRS recover successfully, deaths have also been reported. The reason for this is not well understood. Further research is required to identify predictive biomarkers that could enable early detection of cases where CRS is likely to develop, allowing the most suitable mitigation strategies to be enforced early on before detrimental organ damage occurs.
CAR-related Encephalopathy Syndrome (CRES) is the second most common adverse reaction to ACTs, putting 20-64% of CAR T cell therapy patients at risk.19 Characterized by a neurotoxic encephalopathic state, this comprises symptoms of confusion, headaches, and delirium, with occasional seizures and cerebral edema. The current indicators used in the clinic are not sufficient to predict CRES and its severity. Both CRS and CRES have been observed in patients treated with other T cell redirected therapies including TCR gene therapies, bispecific T cell antibodies (BiTEs), and CAR natural killer cells.19 Other adverse reactions resulting from severe immune activation include fulminant hemophagocytic lymphohistiocytosis (HLH) or macrophage-activation syndrome (MAS) which manifests as an immune-mediated multiorgan failure and lymphohistiocytic tissue infiltration. What makes cell therapy-related toxicity particularly challenging to understand is that the same adverse event may look different in different conditions. For example, a patient with B cell acute lymphocytic leukemia (ALL) suffering from CRES may not exhibit the same symptoms as a B cell Non-Hodgkin Lymphoma patient suffering from the CRES.20 Not only is there a need to stratify patients, but an understanding of the variability in the pathogenesis of these conditions is also required to enable the development of preventative strategies.
The Reduced (or Lack of) Efficacy of Cell Therapies over Time
Amongst patients receiving cell therapies, a reduction in efficacy over time has been observed which is typically accompanied by disease relapse. The reason for the diversity in cell therapy response is not well understood. For example, disease relapse can occur in up to 50% of patients receiving CAR-T cell therapy by month 12 after infusion.19 Contributing factors may include the inability to ensure that these cells persist in vivo and expand to maintain therapeutic effects in the long term. Some cell therapies (e.g., CAR-T) also face the challenge of identifying specific tumor antigens within the tumor microenvironment (TME) due to its heterogeneous antigen expression which makes it difficult to identify and target. The identification of tumor-specific antigens in the TME is necessary to enable the cell therapies to effectively target antigens of tumor cells rather than normal vital tissues. Tumors have also been found to down-regulate oncogenic antigens after treatment with CAR-T cell therapy.21 One could overcome this antigen escape by targeting multiple antigens simultaneously by using, for instance, bispecific CARs with promiscuous receptors (as the antigen-binding portion of the CAR).21
The Impact of the Complex Tumor Microenvironment (TME)
While cell therapies are efficacious for the treatment of liquid tumors (hematological malignancies), their effects in solid tumors are limited due to their inability to penetrate the TME. Understanding cell migration and infiltration to the tumor site remain an important area of investigation with other routes of administration being considered, including intrapleural (e.g., in pleural malignancies) and localized rather than systemic administrations (e.g., intracranial delivery in glioblastoma).21 Another challenge is that the TME exhibits immuno-suppressive properties (e.g., low pH, hypoxia, suppressive factors, and cells that express inhibitory ligands such as PD-L1) which hinder the therapeutic potential of cell therapies by inhibiting T cell activity. Therefore, even if these cell therapies persist and expand in vivo, penetrate the tumor, and recognize tumor cells, their cytolytic abilities (efficacy) may be limited. The biomedical community urgently needs to understand these complex TMEs and identify biomarkers of efficacy and toxicity necessary to implement successful and safe cell therapy treatment regimens.
Moving Towards the Solution
The use of advanced technology such as single-cell RNA Sequencing (scRNA-seq), multiplex immunohistochemistry, and CYTOF (Mass Cytometry), as well as integrating longitudinal gene expression, epigenetics, flow cytometry, and mass spectrometry data could be highly beneficial in understanding cell therapy products, TMEs, and patient responses.21 These technologies of improved sensitivity enable a systems-level approach to better understand complex heterogeneity and gain a comprehensive understanding of patient responses to therapy. Integrating these complex data types is vital yet highly overwhelming. When managing these large amounts of complex and high-dimensional data, it also becomes crucial to have a centralized collaborative space to harmonize, integrate, and analyze such data while maintaining a full chain of custody.
This is exactly why a solution like Genedata Profiler® is key. By enabling streamlined integrative analyses, the software supports patient and donor characterization (e.g., molecular, immune, and clinical) allowing identification of biomarkers of efficacy and toxicity before, during, and after treatment with cell therapies. Using the advanced analytical tools within Genedata Profiler, an improved understanding of cell therapy products, their mechanism of action, and biological targets can be attained. With this platform and the support of Genedata experts, it becomes possible to detect signs of toxicity early to prevent irreversible damage, to match the right donor and cell therapy to the right patient, and ensure these therapeutic products achieve their maximal benefit.
Learn More About Genedata Profiler
Authors:
Marie-Ange Kouassi, Ph.D., Scientific Communication Specialist, Genedata Profiler
References:
- Abraham E, et al. Platforms for manufacturing allogeneic, autologous and iPSC cell therapy products: an industry perspective. New Bioprocessing Strategies: Development and Manufacturing of Recombinant Antibodies and Proteins. 2017.
- Campbell A, et al. Concise review: process development considerations for cell therapy. Stem Cells Translational Medicine. 2015.
- Hutt D. Engraftment, graft failure, and rejection. The European Blood and Marrow Transplantation Textbook for Nurses. 2018.
- Yu H, et al. Dendritic cell regulation of graft-vs.-host disease: immunostimulation and tolerance. Frontiers in Immunology. 2019.
- Scheiner ZS, et al. The potential for immunogenicity of autologous induced pluripotent stem cell-derived therapies. Journal of Biological Chemistry. 2014.
- Osborn TM, et al. Advantages and recent developments of autologous cell therapy for Parkinson’s disease patients. Frontiers in Cellular Neuroscience. 2020.
- Malik NN & Durdy MB. Cell therapy landscape: autologous and allogeneic approaches. Translational Regenerative Medicine. 2015.
- Wang LL, et al. Cell therapies in the clinic. Bioengineering & Translational Medicine. 2021.
- Tarella C, et al. Negative immunomagnetic ex vivo purging combined with high-dose chemotherapy with peripheral blood progenitor cell autograft in follicular lymphoma patients: evidence for long-term clinical and molecular remissions. Leukemia. 1999.
- Karadurmus N, et al. A Review of Allogeneic Hematopoietic Stem Cell Transplantation in Metastatic Breast Cancer. International Journal of Hematology-Oncology and Stem Cell Research. 2018.
- Kuruvilla J. The role of autologous and allogeneic stem cell transplantation in the management of indolent B-cell lymphoma. Blood, The Journal of the American Society of Hematology. 2016.
- Maura F, et al. The role of autologous and allogeneic stem cell transplantation in follicular lymphoma in the new drugs era. Mediterranean Journal of Hematology and Infectious Diseases. 2016.
- Szlauer-Stefańska A, et al. Secondary skin neoplasms in patients after autologous and allogeneic hematopoietic stem cell transplantation procedures. Advances in Clinical and Experimental Medicine. 2020.
- Ratajczak MZ, et al. Pivotal role of paracrine effects in stem cell therapies in regenerative medicine: can we translate stem cell-secreted paracrine factors and microvesicles into better therapeutic strategies? Leukemia. 2012.
- Sharpe ME, et al. Nonclinical safety strategies for stem cell therapies. Toxicol Appl Pharmacol. 2012.
- Kovarik J. From immunosuppression to immunomodulation: current principles and future strategies. Pathobiology. 2013.
- Ryan AE, et al. Chondrogenic differentiation increases anti-donor immune response to allogeneic mesenchymal stem cell transplantation. Molecular Therapy. 2014.
- Frey N, and Porter D. Cytokine Release Syndrome with Chimeric Antigen Receptor T Cell Therapy. Biol Blood Marrow Transplant. 2019.
- Neelapu SS, et al. Chimeric antigen receptor T cell therapy - assessment and management of toxicities. Nat Rev Clin Oncol. 2018
- Wei, J., et al. The model of cytokine release syndrome in CAR T cell treatment for B-cell non-Hodgkin lymphoma. Sig Transduct Target Ther. 2020.
- Srivastava S and R. Chimeric Antigen Receptor T Cell Therapy: Challenges to Bench-to-Bedside Efficacy. Journal of Immunology. 2018.